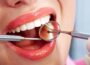
FAT NECROSIS OF THE BREAST

Fat necrosis according to the Lecturio Medical Library is an incendiary, harmless condition coming about because of injury to the breast tissue. Types of injury incorporate obtuse horrendous injury just as injury from surgeries, biopsies, and radiation treatment. Fat rot of the bosom is described by the presence of a poorly characterized bosom mass that is normally joined by overlying skin changes. Oil sores may likewise shape as fibrosis and calcification trap oil from deteriorating fat cells. Fat putrefaction of the bosom might be clinically and radiographically hard to recognize from a dangerous mass. Conclusion depends on a set of experiences predictable with injury, bosom imaging, and, less usually, a center needle biopsy for authoritative analysis. Treatment is normally not needed. The essential clinical meaning of this condition is its conceivable disarray with bosom malignancy on test and imaging.
Definition
Fat rot is a harmless bosom sore that outcomes from injury to the bosom tissue.
The study of disease transmission
Rate: 0.6%
2.75% of all harmless bosom injuries
Normal age at analysis: 50 years
Etiology
Injury:
Direct injury to the chest (counting misuse)
Up to half of patients may not report/review injury.
Fine and center needle bosom biopsies
Surgeries:
Lumpectomy
Bosom reproduction
Bosom decrease
Mastectomy
Free folds
Fat joining
Silicone infusions
Radiation treatment
Mastitis/bosom diseases
Hazard factors:
Huge or pendulous bosoms
More established age
Smoking
Corpulence
Pathophysiology and Clinical Presentation
Pathophysiology
Components of injury:
Slash of bosom tissue blood supply during systems → ischemia → rot
Horrendous drain inside bosom fat tissue
Tissue reaction:
Aseptic saponification:
Unsaturated fats are let out of fatty substances by the blood or tissue lipase.
Unsaturated fats structure a complex with calcium (calcification).
Receptive irritation around saponified tissue brings about fibrosis and scarring.
Another system is cystic degeneration:
Fat cells discharge their substance.
Calcification and fibrosis can conform to the declined fat → oil sores
Clinical show
Firm, sporadic bosom mass (impersonates bosom disease)
Might be delicate, difficult, or effortless
Typically situated in the periareolar region, however may happen anyplace on the bosom
Might be joined by erythema and additionally ecchymosis
Skin or areola withdrawal
Determination
History
Injury (e.g., engine vehicle mishaps, attack)
Bosom a medical procedure/biopsy
Diseases/mastitis
Bosom/chest radiation
Actual test
Careful bosom test:
Firm unpredictable mass, fixed to dermis
Areola withdrawal/skin tying
Axillary lymph hub palpation: Lymphadenopathy might highlight bosom disease.
Imaging
Mammogram:
Discoveries contrast dependent on level of fibrosis.
May show up as a smooth-lined bright mass
May exhibit microcalcifications with spaces of strange murkiness
Ultrasonography:
Less explicit than mammography
Expanded echogenicity of subcutaneous tissue
Hypoechoic, anechoic, or strong mass
Oil sores:
Cystic injuries with echogenic inner groups
Divider calcifications
Bosom attractive reverberation imaging (MRI):
Might be useful in cases with critical fibrosis
Separates fat rot from carcinoma
Fat rot normally seems indistinguishable from nearby fat on MRI.
The board
Perception and consolation
Regular history: Lesions might develop, stay unaltered, or relapse.
Careful administration typically not needed, yet might be picked if the mass:
Doesn’t resolve
Causes torment
Causes bothersome bosom bending
Desire of oil blisters with a needle if the growths cause inconvenience
Differential Diagnosis
Bosom malignancy: the main determination to preclude when a patient presents with a bosom mass or proof of calcifications and fibrosis on imaging, as fat rot might introduce in a very much like manner. On the off chance that the finding can’t be made dependent on imaging alone, center needle biopsy is required. The executives might include a medical procedure, chemotherapy, radiation, and hormonal therapy.
Fibrocystic changes of the bosom: a vague term alluding to a few sorts of harmless bosom conditions that generally happen because of cyclic hormonal incitement from estrogen and progesterone. The most well-known kinds of changes are non-proliferative sores including sores inside the conduits and fibrosis coming about because of constant irritation after these pimples burst. Finding is made with mammogram and ultrasound imaging. Treatment is steady
Mastitis and additionally bosom sore: irritation of the bosom tissue, most generally because of disease with skin or oral verdure presented during breastfeeding. A purulent sore might frame. At times, non-lactational mastitis and abscesses are likewise conceivable. Cases typically present with a fever and torment, erythema, and edema of the bosom, with or without a delicate fluctuant mass (ulcer). The executives includes anti-infection agents, proceeded with articulation of bosom milk if lactating, and cut and waste of a sore.
Galactocele: a cystic assortment of liquid typically brought about by an impeded milk pipe. A galactocele presents as a discernible, firm mass in the subareolar locale and may show an exemplary fat-liquid level on imaging. Determination depends on history and yearning, yielding smooth liquid. These injuries don’t need extraction.
Fibroadenoma: a harmless strong bosom mass made out of sinewy and glandular tissue, which presents as a little, distinct, versatile mass with a rubbery or firm consistency. The specific etiology is obscure. Analysis is affirmed with a center needle biopsy. The executives is either extraction or perception.
Phyllodes cancer: a fibroepithelial growth like fibroadenomas, typically portrayed by quick development. These growths might act like harmless fibroadenomas or may become dangerous and metastasize. Phyllodes cancers are related with Li-Fraumeni disorder. Conclusion is by center needle biopsy and the executives includes total resection, with adjuvant radiation in harmful cases.